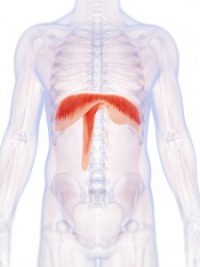
One of the major issues facing persons with quadriplegia/tetraplegia is the need for breathing assistance. While an injury at the C5 vertebrae or lower typically does not affect breathing, injuries above the C4 do often require ventilatory assistance. Individuals with injuries at the C1 and C2 level are totally dependent on assisted breathing. Typically, this has been provided by mechanical ventilators using positive pressure ventilation, though other options are available. The Avery Diaphragm Pacing System is one such option and is typically preferred over traditional mechanical ventilation.
POSITIVE AIRWAY PRESSURE (PAP) VENTILATORS
Mechanical Ventilation is used to permanently or temporarily replace or assist with breathing through artificial means. Traditionally, permanent or temporary mechanical ventilation comes from positive airway pressure (PAP) ventilators. A PAP ventilator will force oxygen into the lungs, and help with the exhalation of carbon dioxide. Though this may help those who cannot breathe effectively on their own, this is not the natural breathing pattern, which utilizes negative pressure to draw air into the lungs.
PAP ventilators rose to popularity in the 1950’s, and became preferred over machines like the iron lung. While they provided advancement in breathing assistance at the time, there are still many drawbacks that are difficult for those needing ventilatory assistance.
First, PAP ventilators are boxy machines that attach via a tracheostomy, or in some cases, via a tube and a mask that fits over the nose and mouth. These may not only be uncomfortable, but may limit mobility and day-to-day activity. Also, the noise level of most mechanical ventilators makes social situations difficult.
In addition, a PAP ventilator does not closely match a person’s natural breathing pattern, which occurs through negative airway pressure. The body normally draws air in; a PAP ventilator will force air in, which many people find uncomfortable.
PAP also carries the possibility of airway injury, ventilator-assisted pneumonia, and collapsed lungs, among other complications.
Financial implications for mechanical ventilation must also be considered. Rental fees and disposable medical supplies associated with mechanical ventilation, for example, are an additional cost. In addition, there may be high costs of frequent hospital stays and readmissions because of ventilator-assisted pneumonia (VAP) and the medications to fight such infections.
OTHER OPTIONS FOR BREATHING ASSISTANCE
PAP ventilators, however, are not the only kind of permanent or semi-permanent mechanical ventilation solutions for those with breathing limitations caused by conditions like high spinal cord injury.
At Avery Biomedical, we provide vent-free breathing that does not require uncomfortable masks or bulky machinery, and we’ve been providing this technology to over 2,000 users for over 40 years.
AVERY BIOMEDICAL’S DIAPHRAGM PACING SYSTEM
Our alternative to traditional mechanical ventilation comes in the form of a surgically implanted device known as a diaphragm pacemaker or phrenic nerve stimulator. This may be considered as an option for anyone who is ventilator-dependent, yet whose diaphragm, lungs, and phrenic nerves have residual function.
The Avery Breathing pacemaker consists of surgically implanted electrodes and receivers with an external transmitter and antennas. The transmitter and antennas send radiofrequency energy to the implanted receivers just under the skin. The receivers then convert the radio waves into small electrical pulses, causing the diaphragms to contract. This contraction causes inhalation of air. When the pulses stop, the diaphragm relaxes and exhalation occurs. Repetition of these pulse trains produces a natural breathing pattern.
Many typically report that the device is much more comfortable as it mirrors a natural breathing pattern and only requires one to carry a transmitter the size of a VHS tape. The diaphragm pacing system typically pays for itself in about 2 years, and represents an average cost savings of $20,000 per year thereafter over mechanical ventilation.
WHAT A DIAPHRAGM PACING SYSTEM MEANS FOR THOSE WITH TETRAPLEGIA
Avery Biomedical’s diaphragm pacing system is surgically implanted through minimally invasive procedures. Additionally, we provide on-site technical assistance to ensure the safe and accurate placement of the diaphragm pacing system.
A diaphragm pacing system more closely mimics the way the body naturally breathes, that is through negative pressure rather than forcing air into the lungs with positive pressure as traditional mechanical ventilators do. This creates a more natural, comfortable feeling. Additional benefits include:
- Decreased risk of infection – Those pacing are at a much lower risk of upper airway infections including ventilator-associated pneumonia due to the reduction in suctioning, elimination of external humidifier and ventilator circuits, and the potential removal of the tracheostomy tube in appropriate cases.
- Increased mobility – Breathing pacemakers are small and do not require the bulky tubing and batteries of mechanical ventilators. Furthermore, unlike PPV, the diaphragm pacing system is silent, increasing the ability to participate in social situations.
- Quality of life – Many with tetraplegia strongly prefer pacing over mechanical ventilation for a variety of reasons including normal breathing and speech patterns, ease of eating and drinking, and improved sense of smell.
- Lower cost – Breathing pacemakers cost far less than the fixed costs and disposable supplies associated with positive pressure ventilation. In addition, diaphragm pacing systems are approved for reimbursement under Medicare, and most private and government insurers worldwide.
NICOLE’S STORY
Nicole was in a car accident when she was 4 years old and suffered a C3/C4 spinal cord injury. As a result, she was on a ventilator for 7 years. She elected to have the Avery Diaphragm Pacing System implanted, and the decision has been life changing. See Nicole’s story below, and what is possible with the help of the Diaphragm Pacing System.
Content reviewed July, 2024 by Dr. Don Headley, M.D.
Dr. Headley is an otolaryngologist (ENT) with almost 40 years of experience in medicine. He is a graduate of George Washington University School of Medicine and Health Science, has been affiliated with St. Joseph’s Hospital and Medical Center in Phoenix, Arizona, and previously served as assistant professor of Internal Medicine and Surgery and Creighton University Medical School in Omaha, NE.

